At A&T Respiratory Lectures, we are dedicated to providing top-tier educational services designed to enhance the skills of healthcare professionals and improve patient outcomes. Our curriculum covers essential topics ranging from advanced mechanical ventilation strategies to patient-focused disease management.
Comprehensive education on using CPAP and BiPAP devices effectively for respiratory support.
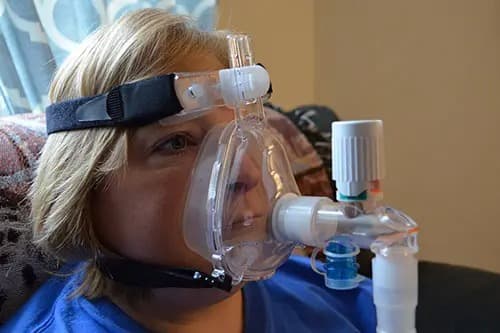
Patient-focused asthma education to improve management and control of asthma symptoms.
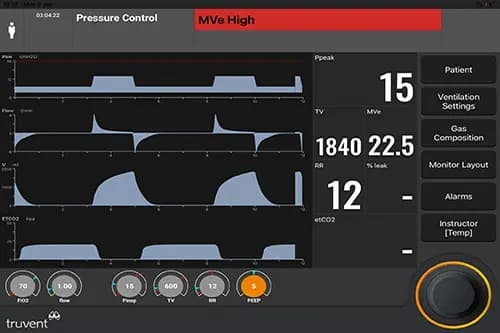
A program designed to improve the well-being and physical condition of patients with chronic respiratory diseases.
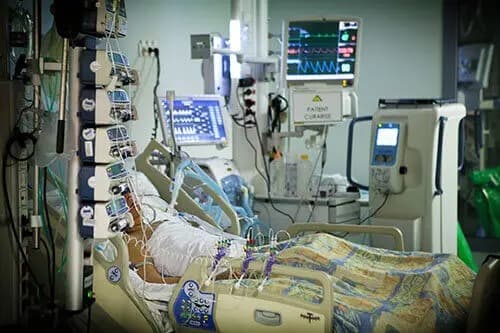
Guidance and support for patients to quit smoking and improve lung health.

Assistance and education on proper oxygen therapy techniques and usage.
